Threat of COVID-19 infection kept millions of Americans from getting routine cancer screenings early in the pandemic. But research indicates screenings still lagged by the beginning of 2021, especially colonoscopies.
A study published in the journal Cancer, which included more than 700 cancer facilities nationwide, found by January 2021 most of those surveyed had not seen screenings rebound to pre-pandemic levels. Colonoscopies dropped by nearly half compared to 2019.
At the same time, new cancer diagnoses dropped 13% to 23%, depending on the type, because fewer cases were being detected.
To help get some Chicagoans back on track and improve health outcomes, Health Care Service Corporation (HCSC) and its Illinois plan recently launched a three-year colon cancer screening initiative at two community centers.
“We can actually prevent cancer from occurring through early screening. We’ve got some catching up to do.”
Located in near some of Chicago’s most underserved ZIP codes, the centers held events where medical experts and colon cancer survivors educated residents about the disease and explained the importance of early screening and diagnosis.
“The audience was very interested in the survivor stories,” says Laron Taylor, community centers director. “They had many questions about the symptoms and were very interested in hearing their experiences with overcoming colorectal cancer.”
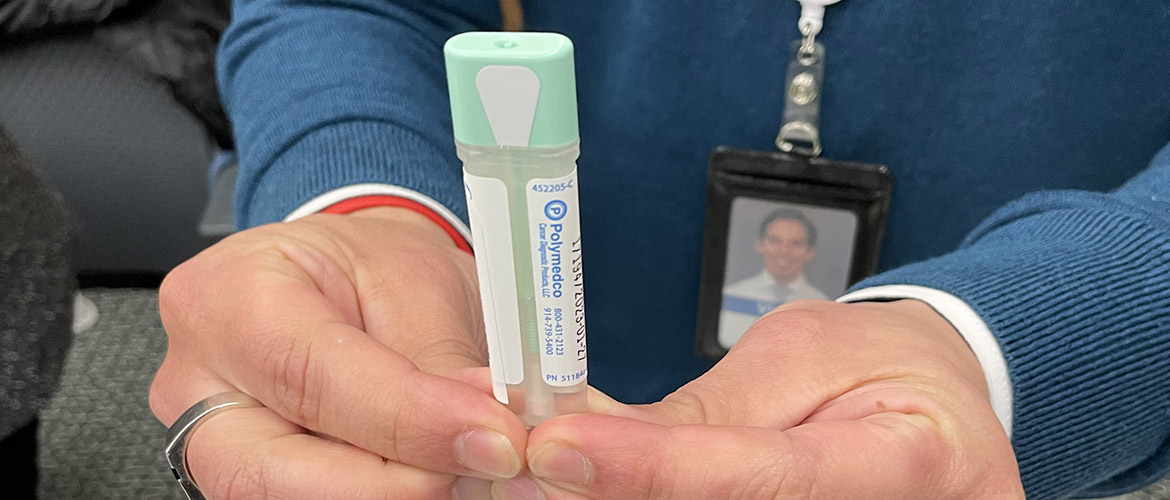
Those who attended the events participated in healthy-cooking and exercise demonstrations. They also were offered free at-home colorectal cancer screening tests, fecal immunochemical test (FIT) kits, an effective and less invasive screening for colorectal cancer.
“We know that in some communities we've seen a disparity in both the incidence of colorectal cancer as well as death rates from colorectal cancer,” says Dr. Derek Robinson, vice president and chief medical officer for the Illinois plan.
“Certainly in the African-American community we see a death rate that is much higher than what we see in other communities," Robinson says. It's really important that we educate people regarding both the things that may place them at greater risk for colorectal cancer as well as updated recommendations to begin screening at age 45 for those of average risk for colorectal cancer.”
Colorectal cancer is the third most common cancer diagnosed in the United States, according to the American Cancer Society. It’s the second most common cause of cancer deaths for men and women combined and expected to cause more than 52,500 deaths this year.
For years, HCSC has offered FIT kits to targeted member populations to screen themselves for colorectal cancer and return them for analysis. After the COVID-19 outbreak forced most Americans to stay home in 2020, HCSC increased efforts to send FIT kits to members and encourage home testing.
With a FIT kit, a stick or brush is used to collect a small stool sample, which is returned to a doctor or lab where the sample is checked for blood — an early sign of colorectal cancer. A colonoscopy is recommended as a follow-up test if a FIT detects blood.
In 2021, the company sent kits to nearly 67,150 individual plan members who were at least 45 years old and had not had a colonoscopy. Results were shared only with the participating members and the primary care provider they identified.
Of the 11,029 members who performed the tests and returned them for analysis, 614 had abnormal results and were encouraged to schedule follow-up colonoscopies.
“Colorectal cancer screening should be on the to do list for everyone,” Robinson says. “We can actually prevent cancer from occurring through early screening. We’ve got some catching up to do.”
Pandemic impacts cancer diagnoses
HCSC claims data suggests the pandemic may have affected screening rates for several cancers. However, company leaders do not anticipate a surge in cancer diagnoses despite a screening lag.
Diagnoses for at least five cancer categories — colorectal, cervical, prostate, lung and breast — plunged almost immediately after the pandemic was declared in 2020. However, diagnoses rates for all five quickly increased as communities eased COVID-19 restrictions and doctor’s offices and clinics reopened to treat more patients.
Dr. Mitch Magee, HCSC’s oncology medical director, says the swift rebound indicates short COVID-related delays didn’t substantially prohibit members from seeking care and probably won’t dramatically affect their treatment. He says research published in the Annals of Thoracic Surgery indicates treatment delays up to three months for some lung cancers did not significantly affect five-year survival rates.
“A delay of a month is not going to make a big difference in the stage of cancer at diagnosis or treatment outcomes going forward,” says Magee, a thoracic surgeon. “Delays are bad, but long delays are worse.”
In 2021, HCSC’s plans in Illinois, Montana, New Mexico, Oklahoma and Texas helped close some gaps by reaching out to nearly 7,550 eligible members and helping them get breast and colorectal cancer screenings.
“We need to ensure that individuals know that it is safe to return to care and do so armed with a screening priority list informed by knowledge of how based upon their age, family history and other risk factors affect their risks for cancer,” Robinson says.